Most doctors do not fear CMS audits because they believe they did nothing illegal.
They fear audits because they know how easy it is to look wrong on paper, even when patient care was correct.
One missing sentence in a progress note.
One modifier is used too often.
One diagnosis code does not clearly support medical necessity.
Months or even years later, CMS asks for records. Payment that felt final suddenly is not final anymore. Refund letters arrive. Cash flow tightens. Staff panic follows.
This is why every medical practice needs a clear CMS audit checklist. Not after an audit starts, but long before it happens.
A CMS audit is not rare. It is not random either. Most audits come from billing patterns, not fraud. Solo practices, group practices, and specialty clinics all face the same risk. High E/M levels, modifier usage, or incomplete documentation can quietly trigger reviews.
This guide is written for U.S. doctors and practice owners. It explains CMS audits in plain language. It shows what CMS looks for, why refunds happen, and how to protect your revenue without changing how you care for patients.
What a CMS Audit Really Means for Medical Practices
A CMS audit is a formal review of your Medicare claims. CMS or its contractors check whether the services you billed were properly documented, medically necessary, and coded correctly.
CMS rarely performs audits directly. Most audits are handled by Medicare Administrative Contractors, often called MACs. These contractors process claims and monitor billing behavior in specific regions of the U.S.
An important point many doctors miss is this. A paid claim is not a protected claim. CMS has the right to review paid claims years later. Payment does not mean approval. It only means the claim passed automated checks at that time.
Audits focus on patterns. CMS compares your billing behavior with peers in your specialty and region. When something looks different, records may be requested.
This is why good doctors get audited. Audits are data-driven, not accusation-driven.
Why CMS Audits Medical Claims
CMS audits claims for three main reasons.
The first reason is medical necessity. CMS wants proof that the service was reasonable and needed for the patient’s condition. Diagnosis codes must support the level of service billed.
The second reason is coding accuracy. CPT, ICD-10-CM, and HCPCS codes must match what was documented. Even small inconsistencies can raise red flags.
The third reason is payment integrity. CMS is required by law to recover overpayments. If documentation does not fully support the claim, CMS considers it an overpayment, even if the care was appropriate.
In real practice, many audits begin after CMS detects repeated use of higher-level E/M codes, frequent modifier 25 usage, or billing patterns that do not align with local coverage determinations.
CMS Audit Types Every Doctor Should Know
CMS audits are not all the same. Understanding the type of audit helps reduce panic and confusion.
A pre-payment audit happens before CMS pays the claim. Payment is delayed until the records are reviewed.
A post-payment audit happens after payment. This is the most stressful type because refunds may be requested.
Targeted Probe and Educate audits focus on specific issues. CMS reviews a small number of claims and provides feedback. These audits are often a warning sign.
Comprehensive audits review large volumes of claims over extended periods. These can lead to significant recoupments.
Knowing the audit type helps practices respond correctly and avoid unnecessary mistakes during record submission.

CMS Audit Documentation Requirements
Documentation is the foundation of every CMS audit. Most audit failures happen here.
CMS expects documentation to clearly show what was done, why it was done, and how it was done. Notes must support the diagnosis, service level, and any modifiers used.
Medical necessity must be obvious. CMS does not guess. If the reason for care is not clearly stated, it is treated as missing.
Progress notes should be complete but focused. Overuse of templates without patient-specific details is a common audit problem. CMS reviewers are trained to spot cloned notes.
Signatures must be present. Missing or late signatures can invalidate otherwise correct services.
Local Coverage Determinations and National Coverage Determinations must be followed. If an LCD limits frequency or indications, documentation must reflect compliance.
In real audits, many refunds occur because documentation is incomplete, not because the service was wrong.

CMS Audit Checklist for Physicians
This CMS audit checklist is designed to protect practices before, during, and after audits.
Before any audit notice arrives, practices should review their most common billed services. High-volume CPT codes should be checked for documentation consistency. Modifier usage should be reviewed for medical necessity support. Diagnosis codes should be evaluated for specificity.
When an audit notice arrives, timing matters. CMS sets deadlines for record submission. Missing deadlines can result in automatic denials.
Only requested records should be submitted. Sending extra records can create new review issues. Documentation should be clean, complete, and organized.
During submission, records should clearly show the link between diagnosis, service, and medical necessity. Review notes as if you are the auditor. If something is unclear, it will be unclear to CMS as well.
After submission, practices should prepare for outcomes. Not all audits end in refunds. Some end with education or partial denials.
This checklist is not about perfection. It is about clarity.
Common CMS Audit Mistakes That Lead to Refunds
Refunds often shock doctors because care was real and necessary. The issue is usually how it was documented.
One common mistake is overusing modifier 25 without separate documentation for the problem-oriented visit. CMS expects a distinct service beyond the preventive visit.
Another issue is high-level E/M billing without enough history, exam, or medical decision-making support. Time-based billing must include total time and qualifying activities.
Diagnosis mismatch is also frequent. The diagnosis billed must justify the service level. Vague or nonspecific ICD-10 codes weaken claims.
Cloned notes raise serious concerns. CMS views identical notes across visits as a lack of individualized care.
These mistakes are rarely intentional. They are workflow issues that grow over time.
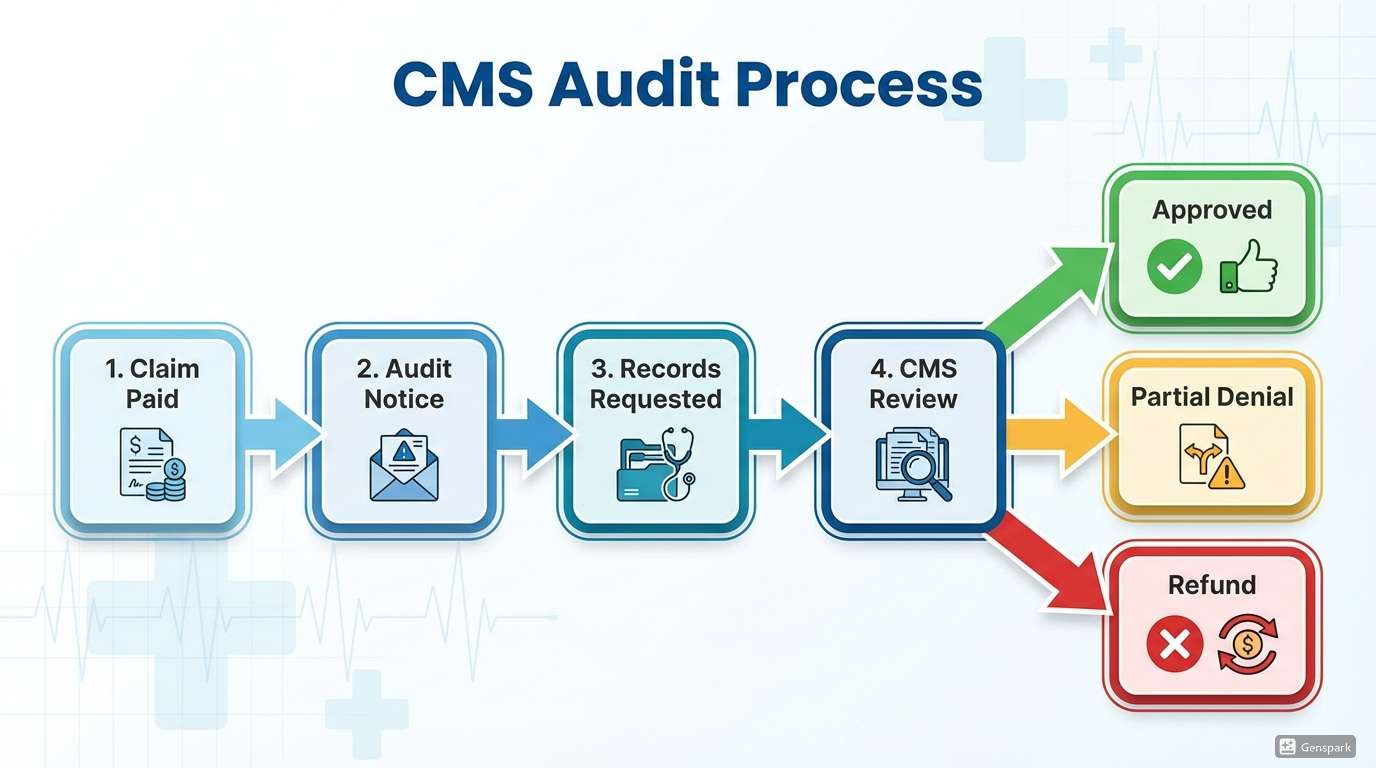
What Happens After a CMS Audit Decision
After CMS reviews records, a determination is issued. Claims may be approved, partially denied, or fully denied.
If overpayments are identified, CMS issues a refund demand. Practices may be required to repay funds or face offset from future payments.
Appeal rights exist. Redetermination and reconsideration levels allow practices to challenge decisions. Deadlines are strict and must be followed.
Many practices lose appeals not because they are wrong, but because the documentation was not strong enough to support the argument.
Understanding the audit timeline helps practices respond calmly instead of reacting emotionally.
How to Prepare for a CMS Audit Before It Happens
Preparation is the best protection.
Practices should perform regular internal reviews of high-risk services. This does not require fear-based auditing. It requires smart sampling.
Billing staff and providers should communicate. Documentation issues often arise when billing expectations are not understood by clinicians.
EHR templates should support compliance, not speed alone. Templates should prompt for medical necessity details without encouraging cloning.
Education should be ongoing. CMS rules change. What passed last year may not pass today.
Prepared practices experience fewer refunds and less stress.

When to Get Professional CMS Audit Support
Some audits require experienced support. Large record requests, complex coding issues, or extended review periods may justify outside help.
Professional audit support focuses on documentation clarity, coding alignment, and compliance strategy. The goal is education, not blame.
Early guidance often prevents small audits from becoming large financial problems.
A CMS audit checklist helps protect your practice revenue. Most audits come from patterns, not fraud. Clear documentation, correct coding, and preparation reduce refund risk. Payment does not mean approval. Preparation matters.


